Lorem ipsum dolor amet, consect adipiscing elit, diam nonummy.
Lorem ipsum dolor amet, consect adipiscing elit, diam nonummy.

The Patient & Carers Race Equality Framework is an accountability framework aimed at eradicating racial bias against Black, Asian, and Minority Ethnic communities in mental health services. It forms a key component of the Advancing Mental Health Equalities strategy, established in 2020. It will provide national expectations to all mental health trusts to fulfil their statutory duties under core legislation.
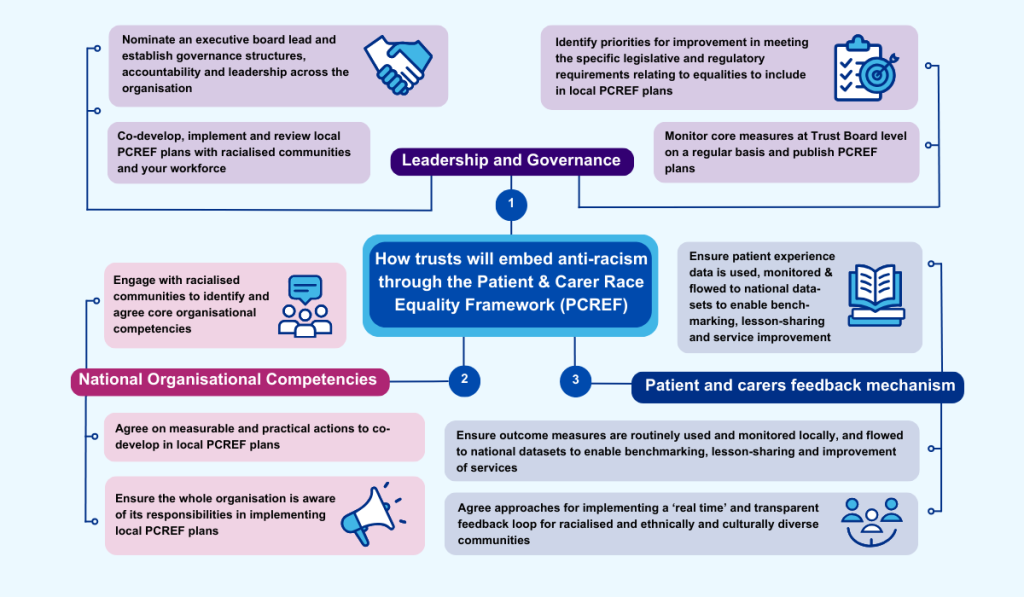
PCREF is a framework based on three core components:
1. Leadership and Governance
PCREF will set out expectations for all mental health trusts to fulfil their statutory duties under core pieces of legislation, such as the Health and Social Care Act, and the Equalities Act.
2. National Organisational Competencies
The competency framework supports trusts to improve patient and carer experience for ethnic minorities. It will help to identify ‘what good looks like’, with examples developed by experts from racialised and ethnically and culturally diverse communities.
3. Feedback Mechanism
PCREF will establish a patient and carers feedback mechanism, to embed patient and carer voice at the heart of the planning, implementation and learning cycle.
Tackling health inequalities is key to improving access to services, health outcomes and improving the quality of services and the experiences of people.
The NHS Long Term Plan has prioritised action on reducing health inequalities requiring every local area in England to develop a detailed plan of how they will reduce health inequalities over the next five to ten years. In addition to the benefit to individuals and society from reducing health inequalities, there is an economic case for action, with the cost to the NHS of ill health resulting from health inequalities being estimated as more than £5.5bn.
There is also a legal duty for NHS England to have regard to the need to reduce inequalities between patients in access to health services and the outcomes achieved (Health and Social Care Act, 2012). In addition, there is a duty to address equality under the Public Sector Equality Duty (PSED) of the Equality Act 2010 to understand the potential effect of policies and practices on people with ‘protected characteristics
Data consistently highlights that people from ethnic minority backgrounds (especially Black backgrounds) are:
PCREF launches in November 2023 across all mental health trusts in the UK. To date, it has been test in pilot programmes across South and East London, Birmingham and Manchester. Drawing on the advice and experiences of the pilot programmes, communities, patients and carers, PCREF is a ground-breaking opportunity to drive race equity into systematic change.
As an example of what PCREF pilot sites have been doing, our partners South London and Maudsley (SLaM) have embedded within their new strategy vision to become leaders of anti-racism. This means that SLaM aim to make substantial progress and eventually to eliminate structural racism in taking demonstrable restorative and equitable actions.
SLaM aim to roll out PCREF activist roles to help raise awareness and support communities to feel empowered and address racial inequalities.
Moreover, all Mental Health Trusts and organisations should hold safe conversations about the impact of racism on the care and experiences of racialised communities and discuss the need to develop anti-racist approaches. This could include:
Reviewing policies and practices to ensure services offered are culturally appropriate and do not leave patients and carers feeling excluded.
Creating a safe place for staff/patients and carers to discuss if they feel impacted by cultural biases which could improve bias of these organisations themselves.

Between 1st April 2021 and 31st March 2022 people were detained 53,337 times under the Mental Health Act.
Amongst broad ethnic groups, known rates of Community Treatment Orders use for the ‘Black or Black British’ group were over eleven times the rate for the White group.
Amongst the five broad ethnic groups, known rates of detention for the ‘Black or Black British’ group were over four times those of the White group.
The launch of the Patient and Carer Race Equality Framework (PCREF) is a significant moment for me. I have been a carer representative on the NHS England PCREF Steering Group since it started over three years ago and I am looking back on 37 years as a carer wondering what could have been different if a PCREF had been in place.
I felt powerless as soon as my brother was diagnosed with paranoid schizophrenia and taken by force into the mental health system. When I asked about therapy I was told that it would not work for him. When I asked about the medication putting him into a zombie-like state I was told that was the only way to control the symptoms. When I asked about the cocktail of physical health conditions there were shrugs. Although he had a degree in economics the idea of him working again was scorned. I was speaking into no listening. The message was that I should not expect a positive result. Ever. It did not occur to me that some of my experiences were racialised. Why would it? The professionals I came across were generally decent and nice enough people (and a few have been really good) and it probably didn’t occur to them either.
It was several years later that I learned that people with severe mental illness were more likely to have physical health conditions and that Black men were much more likely than their White counterparts to experience psychosis, to be taken by force into the mental health system, to be denied therapy and to be over medicated.
So how will the PCREF help?
Trusts collecting, analysing and publishing data by ethnicity should have been happening by law for a few decades but hasn’t been done universally or to an adequate standard. More importantly, there has been no expectation that the pattern of racial differences in access (e.g. to therapy), experiences and outcomes would be shared with staff, patients, carers and voluntary sector organisations so that they have a clear picture of what is happening and be involved in identifying options for learning and improving things. In addition to data on things like access to services, detentions under the mental health act and forcible restraint and medication, the Patient and Carer Feedback Mechanism will support trusts to improve the collection of patient experience data and ask themselves questions about the effectiveness of their care and treatment.
The power of regulators to change the experiences and outcomes of citizens cannot be underestimated. I have often wondered how trusts that showed disproportionately bad outcomes for patients from racialised communities could be judged as good by the Care Quality Commission (CQC). One of the things that has given me most joy from being part of the PCREF Steering Group has been seeing the CQC developing its inspection framework to include attending to the needs of racialised and ethnic minority communities.
The unacceptable situation for racialised communities in mental health services is about “the system” and not about individuals not doing a good job and over the 37 years that I have interacted with the system there is no doubt that things have improved. But not enough by a long way. Borrowing the metaphor from The Water of Systems Change (Kania, Kramer and Senge, 2018), most of us have been swimming in the water of racism without knowing it. I think it is important to recognise that the mental health system is the product and culmination of the racist water that has bathed us from birth and cannot on its own fix everything. Nevertheless, it needs to fix its own stuff. So the PCREF is a systemic response to a systemic problem and my hope is that a healthy anti-racist system will lead to better job satisfaction for health professionals, a sense of being heard for us carers, and most importantly, better experiences and outcomes for those we care for.
(Trigger Warning: The following writing includes a retelling of cultural trauma that involves police brutality and unlawful death.) Written by Danny Danjuma Life on Mental Health wards can be challenging at the best of times, and while regulatory Life on Mental Health wards can be challenging
